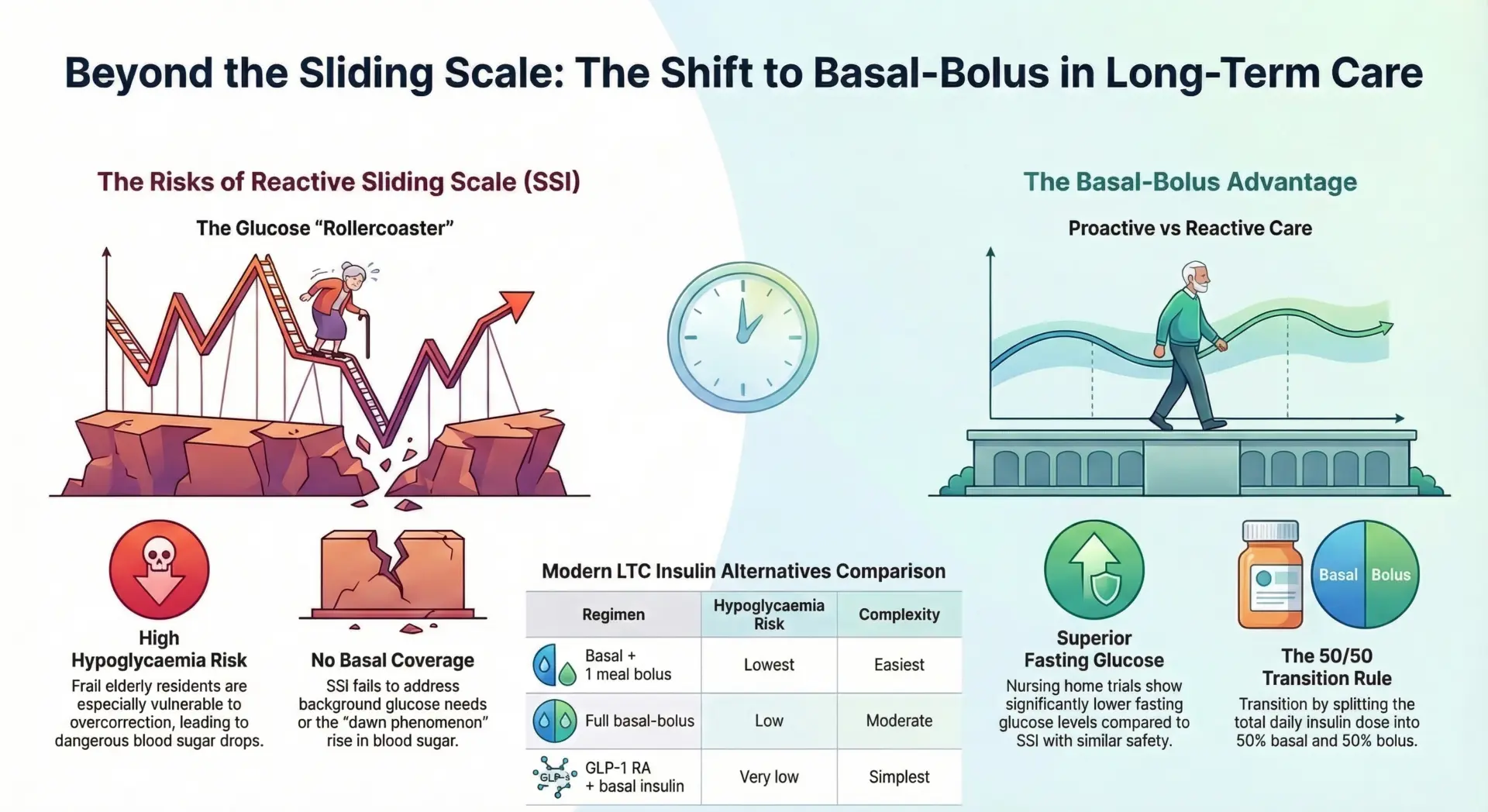
Sliding scale insulin is fading in long-term care because it is a purely reactive approach that treats hyperglycemia after it happens rather than preventing it. This correction-only method doses short-acting insulin based on a patient’s current blood glucose readingtypically before meals and at bedtimewithout providing any baseline (basal) insulin coverage throughout the day.
The result is a “rollercoaster” pattern of glucose spikes and drops that is especially dangerous in frail elderly residents of nursing homes and long-term care (LTC) facilities. Multiple clinical trials and meta-analyses have demonstrated that basal-bolus insulin therapy produces superior glycemic control compared to sliding scale insulin alone.
TL;DR
- Sliding scale insulin (SSI) is losing ground in long-term care because it reacts to high blood glucose after the fact rather than preventing it.
- The ADA 2026 Standards of Care explicitly discourages sole use of correction-only insulin in institutional settings.
- A landmark 21-day randomized controlled trial in nursing homes demonstrated that basal-bolus insulin therapy significantly lowers fasting blood glucose compared to SSI, with comparable safety.
- Modern alternatives including basal-bolus regimens, GLP-1 receptor agonists, and simplified basal-plus-one protocols offer proactive glycemic control, fewer fingerstick burdens and better outcomes for elderly nursing home residents.
What is Sliding Scale Insulin? (And Why It’s Problematic)
Sliding scale insulin therapy is a diabetes management method in which a set of predetermined insulin doses are administered based solely on the patient’s blood glucose reading at the time of measurement.
It uses short-acting or rapid-acting insulin such as regular insulin or Novolog (insulin aspart)given as correction doses when blood sugar rises above a target threshold. Critically, SSI provides no basal insulin component.
It does not account for carbohydrate intake at meals, prior insulin doses already administered, or the patient’s overall insulin sensitivity. This approach has been widely used in hospitals and nursing facilities for decades because of its simplicity for staff to follow, but the evidence against it has grown substantially.
Typical Novolog Sliding Scale Chart Example:
| Blood Glucose (mg/dL) | Novolog Dose (units) |
| 150–199 | 2 units |
| 200–249 | 4 units |
| 250–299 | 6 units |
| 300+ | 8 units (AC + HS) |
Why Sliding Scale Insulin Is Failing in Long-Term Care:
- Glucose “rollercoaster”: SSI creates a cycle of peaks and valleys instead of mimicking the body’s natural physiologic insulin release. Blood glucose levels swing between hyperglycemic episodes and correction-induced drops.
- Higher hypoglycemia risk in frail elderly: Elderly residents with unpredictable nutritional intake are especially vulnerable to overcorrection, placing them at elevated risk of dangerous hypoglycemic events.
- ADA/AMDA 2026 guidance: The ADA’s 2026 Standards of Care state that “sole use of a correction or supplemental insulin without basal insulin in the inpatient setting is discouraged”. Despite these guidelines, roughly one-third of nursing home residents with diabetes are still managed on SSI monotherapy.
- Persistent institutional use: Despite these guidelines, many nursing homes continue using SSI because of staff familiarity and institutional inertia.
- Transition Trigger: LTC facilities should consider transitioning patients off SSI monotherapy when A1C exceeds 8% or fasting blood glucose is above 200 mg/dL on more than half of measured days.
Basal-Bolus vs Sliding Scale: Head-to-Head Data
The strongest LTC-specific evidence comes from Dharmarajan et al.’s 21-day randomized controlled trial conducted across 14 nursing home facilities in the United States.
This AMDA Foundation–sponsored study compared sliding scale insulin monotherapy (control) against basal-bolus insulin therapy (intervention) in 64 nursing home residents with type 2 diabetes mellitus. Participants averaged 80 years of age, and both groups were similar in baseline characteristics.
21-Day Nursing Home RCT Results:
| Metric | Basal-Bolus | Sliding Scale | Winner |
| Fasting BG (end of trial) | Significantly lower | No change from baseline | Basal-Bolus |
| Hypoglycemia (<70 mg/dL) | Similar rates | Similar rates | Equivalent |
| Adverse events | Comparable | Comparable | Equivalent |
The study concluded that basal-bolus therapy produced significantly lower average fasting blood glucose levels after 21 days compared with SSI, while both groups had similar rates of hypoglycemia and adverse events. The authors stated that switching from SSI to basal-bolus therapy is “feasible, safe, and effective in the LTC setting.”
Mechanism: Basal insulin (e.g., Lantus/glargine given at bedtime) prevents the dawn phenomenon and maintains steady background glucose control. Bolus insulin (e.g., Novolog/aspart before meals) covers mealtime carbohydrate loads. This two-pronged, physiologic approach mimics the pancreas’s natural insulin secretion pattern.
Sliding Scale Insulin Chart Problems in LTC
Despite its widespread use, the sliding scale insulin chart carries five fundamental flaws that make it a poor fit for long-term diabetes management in nursing homes:
- Reactive only: SSI treats blood glucose of 250 mg/dL after it happens instead of preventing the spike in the first place. This reactive approach is inherently behind the curve.
- No carbohydrate coverage: A standard sliding scale chart ignores mealtime nutritional intake entirely. A resident consuming 60 grams of carbohydrates at breakfast receives no prospective insulin coverage for that meal. Carbohydrate counting is a far more precise method for determining insulin doses.
- Dawn phenomenon unaddressed: Without basal insulin, fasting blood glucose naturally rises 40–60 mg/dL overnight due to hormonal changes. SSI has no mechanism to manage this.
- Hypoglycemia cascade: Correction doses can overshoot, leading to hypoglycemia. The subsequent rebound and re-correction creates a vicious cycle of glucose instability that places patients at higher risk of both hyper- and hypoglycemia.
- Staff burden: SSI often requires 4–6 daily fingerstick blood glucose tests and corresponding insulin administration, creating a heavier workload for nursing staff compared to basal-bolus protocols that may require fewer daily checks once stabilized.
The AMDA clinical practice guidelines note that SSI monotherapy results in poor glycemic control with a high fingerstick burdenan outcome that neither serves the patient nor the facility’s operational efficiency.
Basal-Bolus Transition Protocol for Nursing Homes
Transitioning from SSI to basal-bolus insulin therapy in a nursing home setting can be performed safely over approximately one week using a structured protocol. Below is a practical conversion framework based on published LTC transition protocols:
Week 1 Safe Switch:
| Timing | Old SSI Regimen | New Basal-Bolus Regimen |
| Bedtime (HS) | Novolog 0–4 units PRN | Lantus 0.1-0.2 u/kg (~10 units) |
| Breakfast | Novolog 2–8 units per scale | Novolog 4 units fixed + 1 unit per 15g carb |
| Lunch/Dinner | Novolog 2–8 units per scale | Novolog 3 units fixed |
| HS Correction | Novolog 1–2 units per 50 mg/dL above target | Same correction scale |
Key Conversion Principles:
Calculate the Total Daily Dose (TDD): Sum the patient’s average daily SSI units over the preceding 3–7 days. Split this approximately 50% basal (Lantus at bedtime) and 50% bolus (Novolog divided across meals).
Hypoglycemia safety net: Hold basal insulin if pre-dose blood glucose is below 100 mg/dL. Reduce the basal dose by 20% if any reading below 70 mg/dL occurred in the prior week.
Titration: Increase basal insulin by 2 units weekly if fasting blood glucose remains above 140 mg/dL. Increase mealtime bolus by 1 unit if pre-meal glucose consistently exceeds 180 mg/dL.
Basal insulin injections are typically taken once or twice per day, first thing in the morning or before bedtime, providing around-the-clock background coverage.
Modern LTC Alternatives to Sliding Scale
The ADA and AMDA recommend a hierarchy of evidence-based insulin regimens for long-term care that moves well beyond the outdated sliding scale approach:
| Regimen | A1C Goal | Hypo Risk | Complexity |
| Basal + 1 meal bolus | 7.5-8.5% | Lowest | Easiest |
| Full basal-bolus | 7.0-8.0% | Low | Moderate |
| GLP-1 RA + basal insulin | 6.5-7.5% | Very low | Simplest |
For many LTC residents, a simplified basal plus breakfast bolus regimen is the most practical first step. It covers approximately 80% of daily glucose excursions while minimizing complexity for nursing staff.
Continuous glucose monitors (CGMs) can further improve diabetes management in LTC by providing real-time blood sugar trends that outperform intermittent fingerstick measurements. Insulin pumps, though less common in nursing homes, represent another option for continuous insulin delivery.
Additionally, GLP-1 receptor agonists (such as semaglutide) combined with basal insulin offer a regimen that carries virtually no hypoglycemia risk an important safety advantage for elderly patients.
Novolog Sliding Scale Chart → Basal-Bolus Conversion
Below is a practical before-and-after example for an 80 kg nursing home resident:
| Old SSI Regimen | Units/Day | New Basal-Bolus | Units/Day |
| Novolog AC/HS scale | 12–20 units | Lantus HS 8U + Novolog AC 12U | ~20 units |
Conversion Steps:
Step 1: Calculate TDD by averaging the patient’s total daily SSI units from the past 3-7 days.
Step 2: Allocate 40-50% of TDD as basal insulin (Lantus at bedtime).
Step 3: Divide the remaining 50-60% equally across three meals as bolus insulin (Novolog before each meal).
Step 4 (Titration): Increase basal by 2 units weekly if fasting glucose stays above 140 mg/dL. Increase meal bolus by 1 unit if pre-meal readings consistently exceed 180 mg/dL.
Your doctor will provide a customized sliding scale insulin chart and basal-bolus conversion plan tailored to each resident’s specific needs, weight, renal function, and nutritional intake patterns.
Implementation Barriers & Solutions
Adopting basal-bolus protocols in LTC facilities faces several practical barriers, but each can be overcome with targeted solutions:
Common Pushback:
- Nursing inertia: “We’ve always done SSI.” Decades of familiarity make change uncomfortable, even when evidence strongly favors new approaches.
- Staff training gaps: Carbohydrate counting and basal-bolus dosing are unfamiliar to many LTC nursing staff trained primarily on sliding scale protocols.
- Cost concerns: The perception that basal insulin (e.g., Lantus) costs more than rapid-acting insulin alone. In practice, total insulin usage is often comparable.
Solutions:
- AMDA-endorsed order sets: Pre-printed or electronic basal-bolus protocols reduce physician order variability and make the transition systematic.
- Kitchen carbohydrate labeling: A brief 15-minute training session for dietary and nursing staff on reading carb labels can be sufficient for implementing simplified insulin-to-carb ratios.
- GLP-1 receptor agonist conversion: For appropriate candidates, switching to a GLP-1 RA plus basal insulin eliminates mealtime injections entirely, reducing nursing workload while improving outcomes.
Citations & Further Reading
- 16. Diabetes Care in the Hospital: Standards of Care in Diabetes—2026 | Diabetes Care | American Diabetes Association
- Sliding Scale Insulin vs Basal-Bolus Insulin Therapy in Long-Term Care: A 21-Day Randomized Controlled Trial Comparing Efficacy, Safety and Feasibility – PubMed
- Randomized study of basal-bolus insulin therapy in the inpatient management of patients with type 2 diabetes (RABBIT 2 trial) – PubMed
- Randomized Study of Basal-Bolus Insulin Therapy in the Inpatient Management of Patients With Type 2 Diabetes Undergoing General Surgery (RABBIT 2 Surgery)
- The American Diabetes Association Releases “Standards of Care in Diabetes—2026”
- Management of Diabetes and Hyperglycemia in Hospitalized Patients – Endotext – NCBI Bookshelf
Disclaimer: This information is intended for general knowledge and informational purposes only and does not constitute medical advice. Always consult with a healthcare professional for personalized guidance.
Written by the Pandameds.com Editorial Team
Our content is created by pharmacy-trained researchers and healthcare specialists and rigorously reviewed by a diverse panel of authentic experts from the pharmaceutical and healthcare fields. This collaborative review process ensures that every article meets the highest standards of medical accuracy, reliability, and relevance.
- ✅ Authored by pharmacy-trained professionals
- 🔍 Reviewed by multiple verified experts in the pharmaceutical and healthcare niche
- 💊 Based on trusted sources including FDA, Health Canada, and peer-reviewed clinical studies
- 🔄 Regularly reviewed and updated every 90 days to maintain accuracy and trustworthiness
About Pandameds.com
Pandameds.com offers a range of weight loss medications at an affordable price.
Fast, Reliable Shipping to the USA!
Affordable Prescription Meds From Canada
Join our mailing list for exclusive promos, curated health content & more.
Frequently Asked Questions
What is a sliding scale insulin chart?
A sliding scale insulin chart is a table with two columns: one listing blood glucose ranges (e.g., 150–199, 200–249 mg/dL) and another listing the corresponding correction doses of short-acting insulin (e.g., 2 units, 4 units). To use it, you check your blood glucose level before meals and at bedtime, find the range that matches your current reading, and administer the listed dose. It provides no basal insulin coverage and does not account for carbohydrate intake
Novolog sliding scale vs basal-bolus?
Clinical trials show that basal-bolus therapy significantly lowers fasting blood glucose compared to Novolog sliding scale alone, with comparable hypoglycemia risk (Dharmarajan et al., 2016; Umpierrez et al., RABBIT 2 Trial). The ADA recommends against long-term SSI use. Basal-bolus therapy is compliant with current ADA and AMDA guidelines.
Is it safe to stop sliding scale insulin in LTC?
Yes. The Dharmarajan 21-day RCT demonstrated that transitioning LTC residents from SSI to basal-bolus insulin is feasible, safe, and effective, with no increase in hypoglycemia or adverse events (JAMDA 2016). The transition should be supervised by a physician and follow a structured protocol with appropriate safety monitoring.
What about sliding scale insulin chart dosage for the elderly?
The ADA 2026 Standards of Care recommend that elderly and frail patients in LTC settings should be managed with basal-bolus insulin or GLP-1 receptor agonists rather than SSI monotherapy. SSI monotherapy is strongly discouraged as a primary, long-term diabetes management strategy for elderly patients due to its inability to adequately control blood glucose and its association with increased glycemic variability.
Regular insulin sliding scale vs Novolog?
Novolog (insulin aspart) has a faster onset of action (approximately 10–15 minutes) compared to regular insulin (approximately 30 minutes), making it slightly more practical for mealtime correction. However, both share the same fundamental reactive flaws when used in a sliding scale–only regimen: neither addresses basal insulin needs, carbohydrate coverage, or the dawn phenomenon. Switching from regular insulin to Novolog on a sliding scale does not resolve the core problems of SSI therapy.
Related Blog Posts
Call Us Today!
If you have any questions, please email our support team at support@pandameds.com or call us toll-free at 1-888-862-1210.