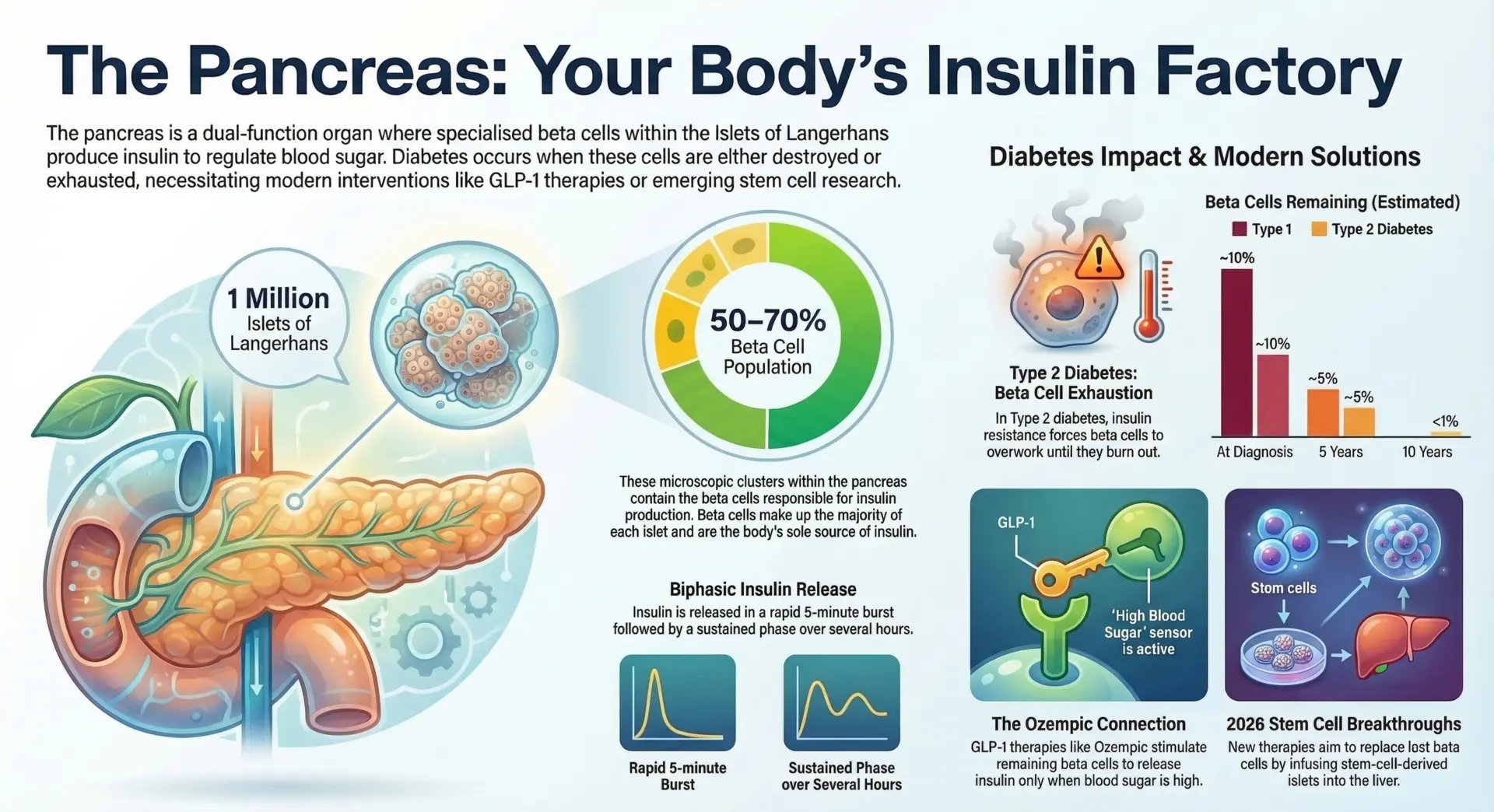
Pancreatitis is a painful condition that causes inflammation of the pancreas and significant damage to the organ. The immune system generally causes pancreatitis, which often leads to swelling and pain.
An inflamed pancreas in the abdomen disrupts its crucial functions of producing digestive enzymes and regulating blood sugar levels through insulin production.
Ozempic (semaglutide) is an FDA-approved prescription medication for Type 2 diabetes. It also helps with weight loss and is found to reduce the risk of major cardiovascular events such as stroke, heart attack or death in adults. However, Ozempic has its set of initial and sometimes serious side effects.
Though the risk is low, there are reports of Ozempic causing acute pancreatitis in individuals. Dawn Gentle, who was taking Ozempic for managing Type-2 diabetes for 3 years straight from 2018 to 2021, experienced the symptoms of acute pancreatitis and was immediately asked to stop Ozempic use.
Symptoms of Pancreatitis
Moderate to severe abdominal pain that radiates to your back is a clear indicator of pancreatitis. Your abdomen may feel tender to the touch. You may notice more pain after meals. Moreover, some people experience constant pain as well.
The other symptoms of pancreatitis include:
- Upper abdominal pain (worsening after eating)
- Nausea and vomiting
- Upset stomach
- Rapid heart rate
- Fever
- Yellowing of skin & eyes
- Loss of appetite
- Weight loss
- Greasy stools
Seek immediate medical assistance if you notice these symptoms right away.
Does Ozempic Cause Pancreatitis? (Rare – <0.1%)
This is one of the most commonly searched questions about Ozempic. The short answer: pancreatitis is a rare but recognized side effect associated with Ozempic and other GLP-1 receptor agonists. However, a direct causal link has not been definitively established.
A 2024 meta-analysis published in Endocrinología, Diabetes y Nutrición analyzed 21 randomized, placebo-controlled trials of semaglutide involving 34,721 patients. The study found that semaglutide therapy was not associated with an increased risk of acute pancreatitis compared to placebo, with an odds ratio of 0.7 (95% CI 0.5–1.2, I² 0%). These results were consistent across oral semaglutide, low-dose subcutaneous, and high-dose subcutaneous formulations.
A larger 2026 retrospective cohort study also found no increased risk of acute pancreatitis in Type 2 diabetes patients using GLP-1 receptor agonists. In fact, a U.S. propensity score-matched analysis suggested that GLP-1 receptor agonist use may actually be associated with a lower rate of pancreatitis compared to non-users.
However, post-marketing surveillance by the MHRA has documented rare cases of severe pancreatitis, including necrotizing and fatal forms. The FDA drug labels for GLP-1 receptor agonists include a warning that acute pancreatitis has been observed, and treatment should be discontinued promptly if suspected.
The bottom line: for the vast majority of patients, Ozempic is considered safe. However, individuals with certain risk factors (discussed below) should exercise caution and maintain close monitoring with their healthcare provider.
Why Ozempic May Trigger Pancreatitis
The exact mechanism by which Ozempic may trigger pancreatitis is not fully understood. However, researchers have identified three leading theories based on current evidence:
- GLP-1-Induced Pancreatic Stress
Ozempic (semaglutide) is a GLP-1 receptor agonist that stimulates the pancreas to release insulin and suppresses glucagon to help regulate blood sugar levels. When this medication is administered to a pancreas that is already inflamed or compromised, it may aggravate the existing condition. The stimulation of GLP-1 receptors on pancreatic tissue could theoretically lead to overstimulation and cellular stress, particularly at higher doses.
- Gallstone Formation and Biliary Complications
Ozempic is associated with gallbladder disease, which is a well-known cause of pancreatitis. GLP-1 medications slow gastric emptying and can affect biliary motility. Combined with the rapid weight loss that often accompanies these drugs, patients may develop biliary sludge or gallstones. These can obstruct the pancreatic duct and trigger an episode of acute pancreatitis.
- Rapid Weight Loss as an Independent Risk Factor
Significant, rapid weight loss regardless of how it is achieved is an independent risk factor for acute pancreatitis. Patients on Ozempic often experience substantial weight reduction, particularly in the early months of treatment. This rapid weight loss can contribute to gallstone formation and changes in bile composition, which in turn can trigger pancreatitis.
A 2025 case series also found that individuals with certain genetic predispositions, such as cystic fibrosis or hemochromatosis, may be more susceptible to GLP-1 agonist-related pancreatitis.
How Common Is Pancreatitis on Ozempic?
For the general population taking Ozempic, the risk of developing pancreatitis is considered very low estimated at less than 0.1%. To put this in context, acute pancreatitis affects approximately 40–50 per 100,000 adults each year in the general population, regardless of medication use.
In clinical trials, the incidence of pancreatitis among semaglutide users was not statistically different from placebo. However, the risk is not uniform across all patients. Certain groups face a higher risk:
| Risk Group | Estimated Risk Level |
| General population on Ozempic | <0.1% |
| Patients with gallstones | ~0.5–1% (elevated) |
| Prior history of pancreatitis | ~2–5% (significantly elevated) |
| Heavy alcohol users | 3x higher baseline risk |
| High triglycerides (>500 mg/dL) | Elevated risk |
The MHRA’s Chief Safety Officer has stated: for the vast majority of patients who are prescribed GLP-1s, they are safe and effective medicines which deliver significant health benefits. The risk of developing severe side effects is very small, but awareness is essential.
How to Prevent Pancreatitis on Ozempic
You can significantly reduce your risk of developing pancreatitis while taking Ozempic by following these evidence-based prevention strategies:
- Be Transparent About Your Medical History
Before starting Ozempic, inform your healthcare provider about any history of pancreatitis, gallstones, gallbladder disease, alcohol misuse, or high triglyceride levels. These are all risk factors that could increase your chances of developing pancreatitis.
- Pre-Treatment Screening Checklist:
- Get a gallbladder ultrasound before starting Ozempic if you have risk factors
- Have your triglyceride levels tested (levels above 500 mg/dL increase pancreatitis risk)
- Disclose all medications you are taking, including azathioprine, thiazides, furosemide, and estrogens
- Stop or significantly reduce alcohol consumption before beginning therapy
- If you are a smoker, discuss a cessation plan with your doctor
Follow the Prescribed Dosing Schedule
Ozempic is typically started at a low dose and gradually increased. This step-up approach helps your body adjust and reduces the likelihood of gastrointestinal side effects that may mask early signs of pancreatitis. Never increase your dose without your doctor’s guidance.
Adopt a Healthy Lifestyle
A balanced, low-fat diet and regular exercise are recommended alongside Ozempic for optimal results. GLP-1 receptor agonists are not a cure for Type 2 diabetes or obesity but can be highly effective when combined with dietary and lifestyle changes.
Avoid Alcohol Completely
Excessive alcohol consumption is one of the leading causes of pancreatitis. Combining alcohol use with Ozempic significantly raises your risk.
Monitor Symptoms Closely
If you experience any new or worsening abdominal pain while on Ozempic, do not dismiss it as a normal side effect. Report all side effects to your physician to determine if they are serious and if the medication needs to be stopped.
When to Call Your Doctor?
It is common to experience temporary side effects when starting Ozempic, as it takes time for your body to adjust to the medication. However, you must consult your doctor immediately if you experience new or worsening abdominal pain or if you experience pancreatitis symptoms.
This will allow for an early diagnosis of your condition and establish whether Ozempic, used for weight loss and managing Type 2 diabetes, is suitable for your biochemistry.
Management of Pancreatitis
The treatment for pancreatitis depends on its severity. To assess its seriousness, your doctor may recommend blood tests, ultrasounds, CT scans, MRIs, stool tests and more. Treatment may also involve hospitalization, pain medication and intravenous fluids.
You must follow the doctor’s instructions for managing pancreatitis, adhering to the dietary and lifestyle changes they recommend and attending all follow-up appointments so that your condition is monitored well.
Ozempic-induced Pancreatitis – Who is most at risk?
- Prior History of Pancreatitis – Individuals with a previous diagnosis of pancreatitis are at an increased risk of developing the condition again with Ozempic use.
- Gallbladder Issues – People with a history of gallstones, biliary colic or other gallbladder problems are at a greater risk of pancreatitis while on Ozempic.
- High triglyceride levels – Elevated blood triglycerides can increase the risk of pancreatitis.
- Alcohol Use – Excessive alcohol consumption is a known risk factor for pancreatitis.
The use of medications such as azathioprine, thiazides, furosemide, estrogens, and certain antibiotics can also increase the risk of pancreatitis when combined with Ozempic.
Final Words From Pandameds.Com
Ozempic is found to pose a pancreatitis risk in individuals who have a pre-existing condition or a history of pancreatitis or gallstones. You must see your healthcare provider immediately if any Ozempic pancreatitis symptoms occur.
For Ozempic to be a game-changer in your fitness journey and yield substantial weight loss results, take it under your doctor’s supervision, accompanied by the recommended lifestyle changes, such as a low-calorie diet and more movement.
Disclaimer: This information is intended for general knowledge and informational purposes only and does not constitute medical advice. Always consult with a healthcare professional for personalized guidance.
Written by the Pandameds.com Editorial Team
Our content is created by pharmacy-trained researchers and healthcare specialists and rigorously reviewed by a diverse panel of authentic experts from the pharmaceutical and healthcare fields. This collaborative review process ensures that every article meets the highest standards of medical accuracy, reliability, and relevance.
- ✅ Authored by pharmacy-trained professionals
- 🔍 Reviewed by multiple verified experts in the pharmaceutical and healthcare niche
- 💊 Based on trusted sources including FDA, Health Canada, and peer-reviewed clinical studies
- 🔄 Regularly reviewed and updated every 90 days to maintain accuracy and trustworthiness
About Pandameds.com
Pandameds.com offers a range of weight loss medications at an affordable price.
Fast, Reliable Shipping to the USA!
Affordable Prescription Meds From Canada
Join our mailing list for exclusive promos, curated health content & more.
Frequently Asked Questions
Can you take Ozempic if you have a history of pancreatitis?
No, Ozempic (semaglutide) is contraindicated for those with a personal or family history of pancreatitis, per FDA labeling. It could trigger acute flare-ups in at-risk patients.
Does Ozempic increase pancreatitis risk with alcohol?
Yes, alcohol raises the risk up to 3x when combined with Ozempic. Avoid alcohol completely to minimize pancreatic stress.
What is the incidence of pancreatitis with Ozempic?
Clinical trials show an odds ratio (OR) of 0.7, indicating no increased risk over placebo.
What are emergency pancreatitis signs on Ozempic?
Fever, yellow skin (jaundice), or severe pain—go to the ER immediately.
Is Ozempic safe after pancreatitis recovery?
Consult a GI specialist first; it's not automatically approved.
Related Blog Posts
Call Us Today!
If you have any questions, please email our support team at support@pandameds.com or call us toll-free at 1-888-862-1210.